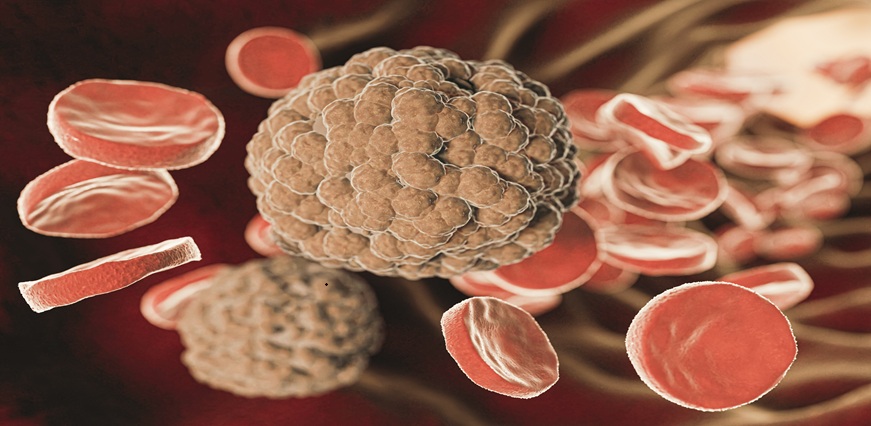
Deep Vein Thrombosis (DVT) is a serious medical condition in which a blood clot forms in a deep vein, most commonly in the legs. It can restrict normal blood flow and, if left untreated, may lead to life-threatening complications such as pulmonary embolism.
The condition often develops when blood flow slows down due to prolonged immobility, certain medical conditions, or the use of medications such as estrogen-based therapies. Common symptoms include swelling, pain, warmth, and redness in the affected area. Understanding the symptoms, causes, and progression of Deep Vein Thrombosis is essential for early detection, effective treatment, and prevention of severe health risks.
What are the Causes of Deep Vein Thrombosis?
The causes of DVT are primarily linked to factors that slow down blood flow or increase the likelihood of clot formation. It typically develops when normal blood circulation is disrupted, especially in the deep veins.
Prolonged immobility such as extended bed rest, long-distance travel, or sitting for long periods, can significantly reduce blood flow and increase the risk of clot formation.
Another major contributing factor is physical damage or pressure on the veins. This may occur due to recent surgeries (especially involving hip or knee), fractures in the pelvis or legs, or the presence of medical devices like catheters.
Certain medical conditions such as cancer, autoimmune disorders, or conditions that increase blood clotting tendency, may also contribute to DVT. Hormonal factors further increase the risk. The use of estrogen-based medications, including birth control pills, particularly when combined with smoking, is associated with a higher likelihood of clot formation.
Additionally, pregnancy, recent childbirth, obesity, and old age further elevate the risk. These factors are often associated with the development of DVT in leg, where clots most commonly occur. Understanding these causes is important, as they are closely linked to early signs of DVT, such as swelling, pain, warmth, and redness in the affected area, which require prompt medical evaluation.
Here are the key risk factors for deep vein thrombosis:
- Prolonged bed rest or sitting in one position for extended periods
- Presence of a pacemaker or catheter inserted through a vein
- Indwelling (long-term) catheter in a blood vessel
- Family history of blood clots
- Fractures in the pelvis or legs
- Recent surgery, particularly involving the hip, knee, or female pelvic area
- Pregnancy or recent childbirth (within the last six months)
- Obesity
- Age above 60
Medical conditions that increase clotting risk:
- Cancer
- Autoimmune disorders such as lupus
- Polycythemia vera (a condition where the bone marrow produces too many blood cells, causing the thickening of the blood)
Lifestyle and hormonal factors:
- Smoking
- Use of estrogen or birth control pills
- Prolonged sitting during travel, especially when combined with one or more of the above factors.
What are the symptoms of Deep Vein Thrombosis?
Common symptoms of Deep Vein Thrombosis include:
- Swelling in one leg, which may develop suddenly or gradually
- Pain, cramping, or a feeling of tightness, usually starting in the calf
- Changes in skin colour, such as redness, purplish tone, or darkening of the affected area
- A warm sensation in the affected area, especially around the swollen or painful region
What are the Stages of DVT?
Generally, there are no classified stages of DVT. Instead, it is understood based on how recent the clot is, how it progresses, and its long-term impact. These classifications are commonly referred to as the stages of DVT, helping in better diagnosis and treatment planning.
- Acute DVT: This refers to a newly formed blood clot, typically within the first few days to four weeks. Symptoms often appear suddenly and may include pain, swelling, warmth, and redness. At this stage, the risk of complications such as pulmonary embolism is higher.
- Subacute or Progressive DVT: If the clot is not managed effectively, it may grow and extend further along the vein, such as moving from the calf to the thigh or pelvic veins. This can lead to long-term issues such as persistent swelling, and a higher chance of complications, including major circulation issues.
- Chronic DVT (Post-Thrombotic Changes): When a clot remains in the vein for more than a few weeks, it may begin to harden or form scar tissue. Over time, this can damage the vein valves, leading to long-term problems like persistent swelling, skin discoloration, and in severe cases, the development of ulcers. This condition is often referred to as post-thrombotic syndrome.
- Recurrent DVT: This occurs when a clot develops again after a previous episode. The risk of recurrence is higher in individuals whose initial clot had no clear cause or in those with ongoing risk factors such as certain medical conditions or blood clotting disorders.
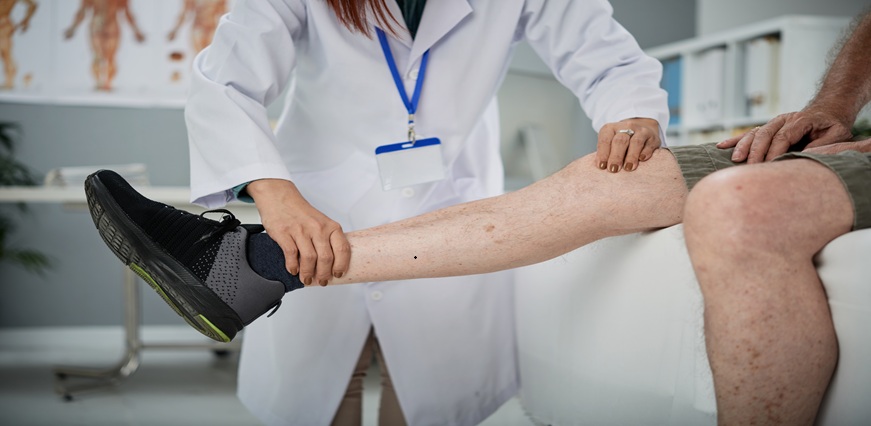
Diagnosis and Tests for deep vein thrombosis
Diagnosing Deep Vein Thrombosis involves a combination of physical examination and specialised tests. Doctors typically assess symptoms such as swelling, pain, and skin changes in the affected area. At Max Lab, advanced diagnostic support helps in the accurate evaluation of such conditions through reliable testing and reporting.
Common diagnostic texts include:
- D-dimer blood test: Measures substances released when blood clots break down
- Duplex ultrasound: A non-invasive imaging test to detect clots and assess blood flow
- Venography: An X-ray test using contrast dye to clearly visualize veins (though used less frequently due to its invasive nature)
- MRI scan: Helps detect clots in deeper or less accessible veins, such as those in the abdomen.
These tests help doctors determine the severity and location of the clot, enabling accurate treatment planning.
Treatment of Deep Vein Thrombosis
The primary goals of treatment are to prevent the clot from growing, reduce the risk of it traveling to the lungs, and minimise recurrence.
Common treatment methods include:
- Blood thinners (anticoagulants): These are the primary treatment and help prevent new clots from forming. They may be taken orally, injected, or given intravenously. Treatment usually continues for at least 3 months.
- Thrombolytic therapy (clot busters): Used in severe cases to dissolve large clots, though they carry a higher risk of bleeding.
- Vena cava filters: Prevent clots from reaching the lungs in specific cases
- Compression stockings: Help improve blood circulation and reduce swelling.
Special care is needed in cases such as DVT in pregnancy, where treatment methods may vary under medical supervision.
Precautions and Tips for Preventing DVT
Taking the right precautions plays a crucial role in preventing DVT and avoiding complications. Recommended measures include:
- Stay physically active and avoid long periods of immobility
- Move or stretch your legs frequently during travel
- Maintain a healthy weight and exercise regularly
- Avoid smoking
- Elevate your legs when resting to improve blood circulation
- Follow prescribed medications carefully
DVT recovery time typically ranges from a few weeks to several months, when managed with proper treatment and lifestyle changes. However, this may often vary depending on the severity of the condition.
Conclusion
Deep Vein Thrombosis is a potentially serious condition that requires timely attention and proper management. From understanding its causes and symptoms to recognising the risk factors and stages, awareness plays a key role in early diagnosis and prevention.
With proper medical care and lifestyle changes, most cases can be effectively managed. Access to dependable diagnostic services, such as those provided by Max Lab, further supports timely detection and informed clinical decisions. Early intervention can help reduce complications, improve recovery outcomes and support long-term vascular health.
































 To reach our help desk call 9213188888
To reach our help desk call 9213188888.png)
Comments