


Home Sample Collection

Highly Trained Staff & Doctors

Same Day Reports Over Email

Zero Contamination QualiCare Kit
No lab centers are available in this city
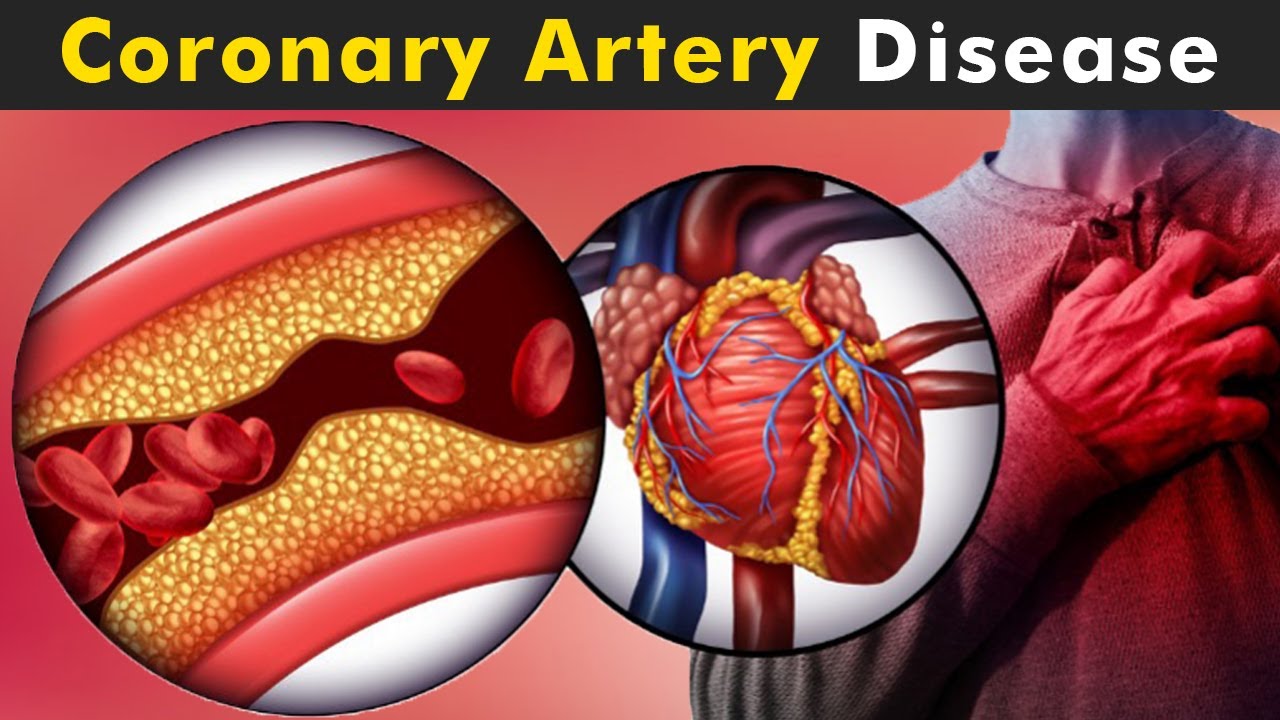
Coronary Artery Disease (CAD) is a common heart condition that affects the coronary arteries which supply blood to your heart. With CAD, plaque build-up narrows or blocks one or more of your coronary arteries. The most frequent symptom is angina (Chest discomfort), which causes chest pain. A heart attack or other consequences like arrhythmia or heart failure can result from CAD.
Coronary Artery Disease (CAD) happens when the coronary arteries that supply blood to the heart become hardened and narrowed, usually due to plaque build-up. This build-up is called atherosclerosis & as it grows, it can lead to less blood passing through the arteries. Angina or a heart attack may result from this. The majority of heart attacks occur when a blood clot abruptly cuts off the heart's blood supply, permanently damaging the heart.
Aside from weakening the heart muscle over time, Coronary Artery Disease (CAD) can also cause arrhythmias and heart failure. Heart failure signifies the heart’s inability to pump blood well to the rest of the body.
One might not even be aware that they have Coronary Artery Disease (CAD) until a heart attack strikes. This makes CAD a "silent killer."
Coronary heart disease (CHD) and ischemic heart disease are further terms for CAD. Additionally, this is what most people mean when they refer to "heart disease" in general.
How does Coronary Artery Disease (CAD) Affect Your Body?
A heart attack is the most common side effect of Coronary Artery Disease (CAD). This is a life-threatening medical emergency. Because it isn't getting enough blood, your heart muscle begins to deteriorate. To revive yourself and restore blood flow to your heart, you urgently require medical care.
Additionally, Coronary Artery Disease (CAD) can weaken your heart over time and cause issues like:
Coronary Artery Disease (CAD) starts when fat, cholesterol and other substances collect on the inside walls of the heart arteries. Atherosclerosis is the name of this condition. The build-up is known as plaque. The arteries may narrow due to plaque, preventing blood flow. The plaque may burst and cause a blood clot.
In addition to high cholesterol, the following factors may harm coronary arteries:
Artery Disease (CAD) is a chronic condition. Plaque build-up might take years or even decades. However, you can experience mild symptoms when your arteries narrow. These signs show your heart is working harder to pump blood—rich in oxygen—to your body.
Symptoms of chronic Coronary Artery Disease (CAD) include:
Stable angina: This is the most common symptom of Coronary Artery Disease. Temporary chest pain or discomfort associated with stable angina appears and disappears in a predictable pattern. Usually, you'll become aware of it when you're engaged in physical or emotional stress. Taking nitro-glycerine (medicine that treats angina) or resting helps in this case.
Shortness of breath (dyspnea): Some people feel short of breath during light physical activity.
Sometimes, the first symptom of Coronary Artery Disease (CAD) is a heart attack. Symptoms of a heart attack include:
Chest pain or discomfort (angina). Angina feels like heaviness, aching, burning, tightness, pressure numbness, fullness or an ache. The shoulder, arm, neck, back or jaw might experience discomfort in the process. Other symptoms include:
Coronary artery disease involves a lot of risk factors. Some are out of your control. Others might be under your control if you make changes in your lifestyle or take medication. The risk factors indicated below and how you can control them should be discussed with your provider.
Non-modifiable risk factors
Age: Your risk of CAD increases as you age. After age 45, the risk is higher for men and those with AMAB. After age 55, the risk increases for women and those with AFAB.
Family history: If any members of your biological family have heart disease, your risk is increased. It's crucial to find out whether they have early heart disease (father or brother before age 55, mother or sister before age 65).
Lifestyle factors that raise your risk
Cardiovascular conditions that raise your risk
Other medical conditions that raise your risk
Through physical test and laboratory tests, healthcare professionals identify Coronary Artery Disease (CAD).
Your doctor will do the following during your physical exam:
Tests that help diagnose Coronary Artery Disease (CAD)
One or more tests may be suggested by your doctor to evaluate your heart's health and identify Coronary Artery Disease (CAD). These consist of:
The same healthy living practices that are used to treat coronary artery disease can also be utilised to prevent it. A healthy lifestyle can contribute to robust, plaque-free arteries. Follow these recommendations to improve heart health:
Depending on the case, your plan may include:
Changes in lifestyle: There's a reason why these tried-and-true strategies feel familiar—they work!
Medication: If making these lifestyle changes isn't enough to improve the health of your heart, you could also need to take medication. Blood thinners (anticoagulants), aspirin and other anti-clotting drugs, ACE inhibitors, beta blockers, nitroglycerin, calcium channel blockers, specific immunosuppressants, statins, or PCSK9s are a few examples of these medications.
Angioplasty: This technique doesn't require opening up your chest and can widen or unblock blocked arteries. Through your blood vessels, a doctor performs angioplasty by guiding a thin, flexible tube with a balloon to the blocked artery. The balloon is then inflated by the doctor, stretching the artery open to allow more blood to flow. To maintain the blood channel open, a small tube known as a stent is frequently also implanted. Usually, you'll spend a day in the hospital and then leave.
Coronary artery bypass grafting: With coronary artery bypass grafting, doctors can circumvent obstructions in your coronary arteries by using blood vessels from other parts of your body.
 Allergy Test
Allergy Test
 Anemia Test
Anemia Test
 Auto immune
Auto immune
 Blood disorder
Blood disorder
 Cancer Screening Test
Cancer Screening Test
 Cancer Test
Cancer Test
 Cardiology Test
Cardiology Test
 Dengue Test
Dengue Test
 Depression
Depression
 Diabetes Test
Diabetes Test
 Fatigue
Fatigue
 Female Cancer
Female Cancer
 Fever Test
Fever Test
 Full body
Full body
 Gastro Test
Gastro Test
 Gastrointestinal
Gastrointestinal
 Gynaecology Test
Gynaecology Test
 Heart Test
Heart Test
 HIV Test
HIV Test
 Hormone Test
Hormone Test
 Hypertension
Hypertension
 Immunity Test
Immunity Test
 Infectious Disease
Infectious Disease
 Infertility Test
Infertility Test
 Influenza Test
Influenza Test
 Iron Test
Iron Test
 Kidney Test
Kidney Test
 Liver Test
Liver Test
 Lung Test
Lung Test
 Nephrology
Nephrology
 Obesity
Obesity
 Orthopedics Test
Orthopedics Test
 Physician
Physician
 Pollution Health Checkup
Pollution Health Checkup
 Pregnancy Test
Pregnancy Test
 Prostate Test
Prostate Test
 Senior Citizen Test
Senior Citizen Test
 STD Test
STD Test
 Thyroid Test
Thyroid Test
 Tuberculosis Test
Tuberculosis Test
 Vitamin Test
Vitamin Test
 Women Health Test
Women Health Test
Get a Call Back from our Health Advisor
New User?
Sign up takes less than 60 secs and gives you access to your offers, orders and lab tests.
Looks like you are not registered with us. Please Sign up to proceed
OTP will be sent to this number by SMS
We have successfully received your details. One of the agents will call you back soon.
 To reach our help desk call 9213188888
To reach our help desk call 9213188888
No Lab Centers are available in this city
Looks like you are not registered with us. Please Sign up to proceed
OTP will be sent to this number by SMS
Not Registered Yet? Signup now.Looks like you are not registered with us. Please Sign up to proceed
Max Healthcare
As a valued member of the Max family, enjoy special discounts every time you book a test.
All Routine
Tests
Additional 10% off on
Wellwise & Max Care Full Body
Discount auto-applied at cart · Cannot be clubbed with other offers






.png)