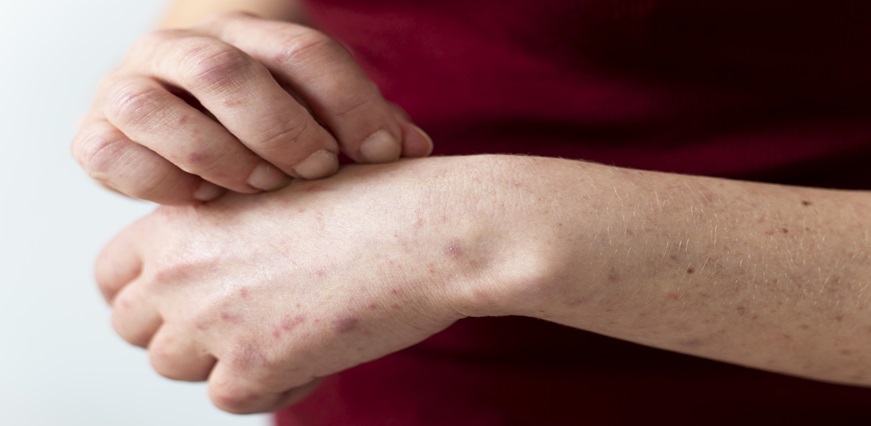
Purpura refers to discoloured patches on the skin or mucous membranes that result from bleeding under the tissue. They appear as reddish-purple spots on light skin and brownish-black on darker skin. This leaked blood pools under the skin, forming noticeable spots or bruises. The discolouration comes from the blood trapped in the tissues just under the surface rather than an external injury.
The meaning of Purpura is any condition characterized by purple or red discolourations on the skin due to bleeding underneath the skin, often caused by small blood vessel ruptures. While not a condition itself, purpura can result from drug interactions, nutritional deficiencies, or hereditary disorders.
Different types of purpura exist based on the underlying cause of the bleeding. Being skin discolouration due to blood trapped beneath the surface, the purpura may indicate a more serious issue, so bruising or spots should be evaluated by a doctor. Proper diagnosis of the cause is important, as the type of purpura determines appropriate treatment.
Types
The different types of purpura relate to platelet counts in the blood. Platelets are cell fragments that form clots to stop bleeding. The two main categories of purpura are:
- Thrombocytopenic purpura - Low platelet levels in the blood
- Nonthrombocytopenic purpura - Normal platelet levels
Thrombocytopenic Purpura (TP)
Thrombocytopenic or Thrombo Purpura (TP) occurs when an abnormally low platelet count (thrombocytopenia) impacts the blood's ability to clot properly. This makes excessive bruising and bleeding more likely. Some potential causes of TP are autoimmune disorders, bloodstream infections, medications that inhibit platelet production, and certain viral illnesses. Boosting platelet production and transfusion may help manage TP symptoms.
Nonthrombocytopenic Purpura (NTP)
In nonthrombocytopenic purpura, platelet levels are normal, so inadequate clotting is not the cause. Instead, other issues like fragile blood vessels, inherited conditions, trauma, medications, ageing, or clotting disorders can produce bleeding under the skin. When platelet counts are normal but purpura still occurs, the cause is some other factor making vessels prone to leakage.
Purpura Symptoms
The symptoms of purpura rash can vary from person to person.
Thrombocytopenic Purpura Symptoms
In thrombocytopenic purpura (TP), low platelet counts result in purple, red or yellowish spots on the skin or mucous membranes like inside the mouth. TP arises from thrombocytopenia when platelet levels drop abnormally low. Other bleeding-related symptoms may accompany TP, without exaggeration:
- Prolonged bleeding from minor injuries
- Blood in urine or stool
- Heavy menstrual bleeding in women
- Unexplained or frequent nosebleeds
- Bleeding gums
- Tiny reddish-purple dots called petechiae
Nonthrombocytopenic Purpura Symptoms
In nonthrombocytopenic purpura, reddish-purple or brownish spots and patches under the skin arise from inflamed or damaged blood vessels or an associated condition, not inadequate platelet levels. Symptoms of purpura vary based on the cause, potentially including:
- Leakage of blood under the skin resulting in discoloured splotches
- Tenderness, burning or itching around purpura spots
- Purpura clustered in gravity-dependent areas like ankles or back
- New spots appearing daily or in different locations
Symptoms may resolve on their own, but some individuals with Henoch-Schönlein purpura or HSP disease may suffer from dangerous inflammation leading to kidney problems.
What Causes Purpura?
Purpura, or the appearance of purple spots on the skin, can have various underlying causes.
Causes of TP include:
- Immune thrombocytopenic purpura (ITP) is an autoimmune disorder where the immune system attacks platelets, leading to a low platelet count and purpura. This increases the risk of bleeding.
- Thrombotic thrombocytopenic purpura (TTP) is a rare condition where small blood clots form, lowering the platelet count and causing purpura. TTP requires prompt treatment.
- Some medications like blood thinners and chemotherapy drugs can reduce platelet counts as a side effect, resulting in purpura.
- Meningococcemia is a bacterial blood infection that can occur when Neisseria meningitidis bacteria spread to the blood. This infection requires urgent antibiotic treatment.
- Autoimmune disorders like systemic lupus erythematosus have also been associated with the development of purpura in some cases.
Nonthrombocytopenic Purpura (NTP) Causes
Nonthrombocytopenic purpura (NTP) involves the appearance of purpura when platelet counts are normal. Contributing factors can include:
- Skin ageing, leading to thinner skin and more delicate blood vessels
- Viral infections such as cytomegalovirus, rubella or Epstein-Barr virus
- Inflammation of blood vessels
- Some medications like corticosteroids
- Certain blood clotting disorders
- Vitamin C deficiency
Diagnosis
To diagnose purpura, a healthcare provider performs a physical exam and closely inspects the skin spots to confirm if they are purpura. They will then review your medical history and any other symptoms before recommending diagnostic tests to help determine the underlying cause.
Important diagnostic tests may include:
- A complete blood count to check levels of blood cells and platelets.
- A skin biopsy to examine a small sample of affected skin under a microscope.
- In some cases, a bone marrow test may be done to evaluate platelet production.
Finding the contributing cause of purpura through selective medical testing can help guide appropriate treatment for purpura. Careful evaluation is important, though testing is focused only on areas directly relevant to the patient's specific presentation and medical background. Ongoing monitoring with the healthcare team ensures the best management.











 7982100200
7982100200























 To reach our help desk call 9213188888
To reach our help desk call 9213188888.png)
Comments